Abstract
Introduction
Myelofibrosis (MF) is a myeloproliferative neoplasm characterized by marrow fibrosis, extramedullary hematopoiesis, and leukoerythroblastosis. Clinical manifestations include severe anemia, splenomegaly, and symptoms. Median survival in patients with primary MF ranges from 2 to 11 years, depending on risk categorization. The National Comprehensive Cancer Network (NCCN) Clinical Practice Guidelines recommend the International Prognostic Scoring System (IPSS) for risk stratification at diagnosis; other systems including the Dynamic IPSS (DIPSS) and the DIPSS-Plus are also cited in the Guidelines. Treatment recommendations are risk-adapted in the NCCN Guidelines. The objective of this study is to describe how patients are risk stratified at diagnosis by community hematologists/oncologists and the impact that risk stratification has on the initiation of MF-directed treatments.
Methods
Medical chart reviews were conducted at community hematology/oncology practices in the OPEN network. Adult patients diagnosed with primary MF, post-PV MF, or post-ET MF between 1/2012 and 12/2016 and receiving care for at least 6 months were included. Data were collected with an electronic case report form (eCRF) with questions on clinical characteristics (symptoms, Hgb, WBC, blast %, and PLT) and risk assessment method used at diagnosis (IPSS, DIPSS, or DIPSS-Plus), treatments, and outcomes. A data-derived IPSS risk score was calculated for each patient. To assess the accuracy of the assigned risk, a data-derived risk score, corresponding to the system used by the provider, was also calculated. Patients were classified as treated at diagnosis if they received MF-directed therapy (hydroxyurea, interferon, ruxolitinib, or clinical trial) or allogeneic hematopoietic cell transplant (HCT) within 120 days of diagnosis. The methods and rates of risk stratification, accuracy of the provider-assigned risk versus data-derived risk, and treatment administered were reported.
Results
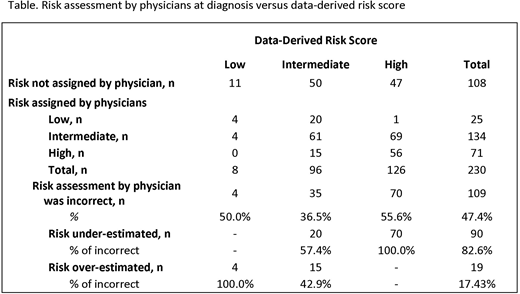
A total of 338 patients with MF from 28 community hematology/oncology practices were included. Mean (SD) age at diagnosis was 65.3 (11.8) years, 51.8% were male, and 68.3% had primary MF. JAK2, MPL, and CALR mutations were tested in 86.1%, 70.1%, and 60.9% of patients at diagnosis, of these, 71.1%, 23.2%, and 14.6% were positive, respectively; 18.4% (38/206) were triple negative. Median follow-up from diagnosis was 27.5 months (IQR, 18.5-42.6). Approximately 32% of patients did not have a risk classification in their medical records at diagnosis. A scoring system was used for risk assignment in 45.3% of patients; DIPSS (23.0%) and IPSS (21.3%) were most commonly used. Of all 338 patients, the corresponding data-derived risk classifications were: 5.6% low, 20.1% int-1, 18.3% int-2, and 55.9% high risk. Among those patients who were not assigned risk by their treating physicians (n=108), most had int-1 (28.7%), int-2 (17.6%), or high risk (43.5%) disease based on the data-derived IPSS risk classification. Of those who received a risk classification from their treating physician, 47.4% (n=109) received an inaccurate risk classification; among these patients, the risk was under-estimated for most (82.6%) (Table 1).
Overall, 55.8% of patients (63.2% low-risk, 55.9% int-1, 52.5% int-2, 56.1% high-risk) received MF-directed pharmacological treatment or HCT within 4 months of diagnosis. Among all patients receiving MF-directed treatment, the mean time from diagnosis to treatment initiation was 5.3 months (SD=1.8), and the most common first pharmacological treatments were ruxolitinib (49.8%) and hydroxyurea (46.7%). Splenomegaly (81.3%), symptoms (72.6%), and anemia (65.6%) were top cited indications for treatment initiation. The treatment initiation rate was higher among those patients correctly risk classified compared to those incorrectly classified (64.2% versus 49.5%, p=0.032).
Conclusions
Nearly one-third of patients with MF did not receive a risk classification at diagnosis. When risk was assigned, almost half were incorrectly classified. Just over half of patients received treatment within four months of diagnosis. Patients who were correctly risk classified at diagnosis were more likely to start treatment promptly upon diagnosis versus those incorrectly risk classified, which may be attributable to the under-estimation of risk.
Verstovsek:Celgene: Membership on an entity's Board of Directors or advisory committees; Incyte: Consultancy; Novartis: Membership on an entity's Board of Directors or advisory committees, Research Funding, Speakers Bureau; Italfarmaco: Membership on an entity's Board of Directors or advisory committees. Yu:Incyte Corporation: Employment, Equity Ownership. Kish:Cardinal Health: Employment. Paranagama:Incyte: Employment, Equity Ownership. Kaufman:Cardinal Health: Employment. Chung:Cardinal Health: Employment. Grunwald:Genentech: Research Funding; Incyte Corporation: Consultancy, Membership on an entity's Board of Directors or advisory committees, Research Funding; Agios: Consultancy, Membership on an entity's Board of Directors or advisory committees; Janssen: Research Funding; Alexion: Consultancy, Membership on an entity's Board of Directors or advisory committees; Celgene: Consultancy, Membership on an entity's Board of Directors or advisory committees; Medtronic: Equity Ownership; Pfizer: Consultancy, Membership on an entity's Board of Directors or advisory committees; Cardinal Health: Consultancy, Membership on an entity's Board of Directors or advisory committees; Amgen: Consultancy, Membership on an entity's Board of Directors or advisory committees, Research Funding; Merck: Consultancy, Membership on an entity's Board of Directors or advisory committees; Ariad: Consultancy, Membership on an entity's Board of Directors or advisory committees; Forma Therapeutics: Research Funding. Colucci:Incyte: Employment, Equity Ownership. Mesa:UT Health San Antonio - Mays Cancer Center: Employment; NS Pharma: Research Funding; Promedior: Research Funding; Gilead: Research Funding; Incyte Corporation: Research Funding; CTI Biopharma: Research Funding; Genentech: Research Funding; Celgene: Research Funding; Novartis: Consultancy; Pfizer: Research Funding.
Author notes
Asterisk with author names denotes non-ASH members.
This icon denotes a clinically relevant abstract